
An interview with Hannah Sail who shares her experience of midwifery and aspirations for the profession, mums-to-be and her career.
Hannah Sail* says being a midwife is who she is but she knew having to return to regular hospital night shifts after seven years of being a community midwife, due to both staff shortages and the planned implementation of the Continuity of Carer policy, would not work for her.
Hannah, now 33, felt she had no option but to leave the Surrey midwifery team she loved in autumn 2022, after eleven years in the profession.
Her eyes well up as she sits in her Worthing flat’s front room, with the sun streaming in the huge bay windows from the direction of the Sussex coast a short walk away.
Embarrassed, Hannah says: “I just feel so sad and guilty.” She pauses for a while and takes a deep breath. “I’ve had to leave what I love when I know there are women I could make a difference to.”
But these are difficult times for midwifery. Hannah has walked away from a profession which is really struggling. There is a shortage of about 2500 midwives and it was recently revealed that maternity has the worst safety ratings of all hospital services inspected by regulator the Care Quality Commission.
Why Hannah was drawn to midwifery

Hannah’s interest in medicine was piqued at 13 when she visited her uncle and aunt – a doctor and a researcher – in India where they provided healthcare to rural families who would otherwise have none. She also recalls her admiration for paramedics who revived a man who collapsed on Worthing beach when she was in her late teens, working as a lifeguard.
Whatever the roots of her interest, she jumped at the chance of shadowing her friend’s mum – a midwife on a labour ward – the same year. Seeing two deliveries made a lasting impression. What really excited her was the special relationship between the midwife and the woman giving birth at such a significant moment in the woman’s life.
She had found her vocation. Hannah started training at a London university in 2011 and, until recently, had no reason to question her decision or her midwifery career.
Hannah’s experience of a struggling maternity service
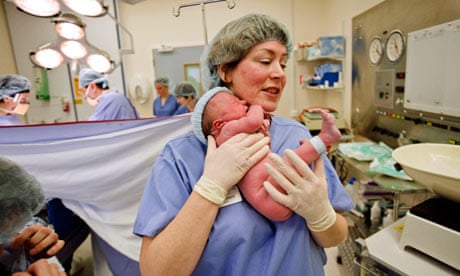
The partially implemented Continuity of Carer policy means, in some cases, midwives have to work in teams of about six with a caseload of women. Between them, they do all the antenatal, delivery and postnatal care, with each midwife likely having to work both on a ward and in the community, across day and night shifts.
Hannah can understand how the policy is beneficial for women giving birth. But in the context of staff shortages and a service under pressure, it is the last straw for some midwives — with her and others having taken a step back from the profession.
When Hannah previously worked on the delivery unit, it took its toll. She couldn’t face returning to that life again. “Doing the night shifts and rotating from one ward to the next due to there not being enough staff, I was feeling really unsettled and my mental health suffered.” She’d often come home crying and felt permanently jet lagged.
“There are many occasions you never get a break,” she says. “You’re on your feet 12 hours and have to be fully focused. Sometimes you can’t even go to the toilet because there’s no one to relieve you. At the ‘time of the month,’ it can be very unpleasant.”
Often hungry, due to there being no staff to cover her so she could have lunch, she’d grab some biscuits before running back in the delivery room with a poker face. It was unsustainable. She took up cold-water swimming in the sea just to keep functioning.
She continued working on the delivery unit for a couple of years and then moved into community midwifery, providing antenatal and postnatal care to women. After seven years in the role, she reached the top level she could without moving into a management position.
During the pandemic, Hannah adapted to working more shifts on the postnatal ward alongside her community midwifery role. The NHS trust ensured those were day shifts so they didn’t detrimentally impact her ability to provide a community midwifery service.
However, with staff shortages and the Continuity of Carer policy, it doesn’t look likely this daytime-only shift pattern will be an option. “I didn’t want to walk away,” she says, “but I felt I needed to.”
Since taking a step back from midwifery to work as an immunisation nurse, she doesn’t feel the need to put herself through cold-water sea swimming anymore.
“I’m living a better life. I enjoy classes in the evening. I go to the beach.” So the question is: “how do I practice midwifery but still stay healthy? That’s my goal.”
Ending NHS bursaries has impacted who’s training to be a midwife
In the context of a notable decline in maternity services and limited staff resources, the NHS needs to attract and retain all the midwives it can. However, since NHS bursaries were stopped in 2017, Hannah says it’s really changed who’s coming onto the degree.
“We’re getting fewer mums and older people coming onto the course because they have children to look after or don’t have the funds to put themselves through university, even with a student loan. It’s a huge loss. All that life experience someone would have benefitted from.”
With a wise head on her shoulders, a dynamic manner and an excellent way with people, Hannah also has a lot of life experience to offer. Along with not having to work nights in an under resourced environment, she wanted to move into community midwifery because it’s so important.
Better preparing women for the first few weeks of motherhood

“Postnatal care is where women need much more support mental health wise,” she says. “People often talk about what’s happened in their delivery, and how traumatic or good it’s been, but no one really talks about the first few weeks after you’ve taken your baby home.
“I think there is a bit of a gap where women are not really prepared for what’s going to happen. Maybe delivery wise but I think we need to realise as a profession what the impact is on women once they’ve delivered their baby.”
This would help to reduce pressure on the scandal of already scarce postnatal mental healthcare.
In her memoir of motherhood and madness, Catherine Cho lucidly shows how the visceral experience of having a baby and the challenges of the postnatal period — having a new life to care for when you may be feeling at your most vulnerable — can trigger past traumas.
Hannah and her colleagues have often chatted about how they’d love to redesign postnatal wards to better support mums after giving birth.
On her home visits many new mums will say: “Oh, that postnatal ward. They will talk about that more than the delivery sometimes, and how it affected them.”
“It’s not really designed to be a healing place,” Hannah says. “Postnatal wards, across every hospital I’ve worked in, have always been the trickiest ward for mums and midwives. But especially for mums.
“I suppose what’s needed is to combine the birthing unit approach that is centred around supporting mum and baby, even if medical monitoring and intervention is required.”
Hannah is clearly passionate about midwifery and supporting women at such an important time in their life. It’s certainly a loss to the profession that she felt she had no option but to leave.
When asked about the future, Hannah hopes to return to midwifery once resourcing, policy and management requirements make that possible in a way that doesn’t put her own health at risk and that ensures the best standards of care for mothers and babies. “In 2024,” she says, “is that really too much to ask?”
*This piece is based on an anonymised interview. Identifying details have been changed to protect the person’s privacy. The core story is real, and shared with deep respect and gratitude for all midwives working under intense pressure.